Understanding CPL
- stacylpearsall

- Jul 11, 2023
- 23 min read
Updated: Jul 25, 2023

Article by Stacy Pearsall
This article explores and outlines existing Chronic Progressive Lymphedema draft horse studies and what one new, promising study means for treatment evolution of CPL.
A horse with CPL does not mean the end of their working life. As long as they are sound and comfortable, they can do just as well as a non-CPL horse, says Hannah Johnsen of www.chronicprogressivelymphoedema.com.
Buckle up and have your dictionary handy, ‘cause this article is a doozy filled with medical terminology. While I’ve done my best to translate it into lay terms, some jargon just doesn’t convert well. Also, I would like to preface this write-up by saying I’m not a DVM or authority on equine health. Like so many, I’m learning as I go and everything you’re about to read is sourced from over 100 published studies, research literature, theories and a smattering of draft horse community forums. I’ve done my best to boil down and simplify (but not over-simplify) the information so you can get an overview of what CPL is and how it impacts the Belgische Trekpaard; hereafter referred to by its American name, the European Brabant or “Brabant” for short. I’ve also included current treatment plans used by a variety of draft horse owners and have highlighted a promising 2022 study conducted by Dr. Marieke Brys, who is the author of “Chronic Progressive Lymphedema in Draft Horses: ‘Mites or Myth?’” and "Chronic Progressive Lymphedema in Belgian Draft Horses: Understanding and Managing a Challenging Disease." Please be sure to see the comprehensive list of all my references at the end of the article for a further deep-dive of your own.
Okay, let’s dive in. Despite numerous aforementioned studies directly, or loosely, related to CPL, there's a lot we still don’t know. Much of what we do know, or what has been circulated amongst the draft horse community, is based on these research studies, some recent and others that are nearly twenty years old. These studies are often laser focused mainly on, but not limited to, genetics, skin and lymph. Some researchers theorize CPL is due to heavy bone and feathering, but even lightly boned and feathered draft breeds have CPL. Many suggest it’s based in genetics and while geneticists identified a whole-genome scan for Chronic Pastern Dermatitis (CPD) in 2009, they have not yet identified a “CPL” gene. Most folks theorize CPL is multifactorial and speculate it’s brought on by the chain reaction of genetic predisposition, mite infestation, skin sensitivity, prolonged inflammatory immune response, living conditions, lack of exercise, diet, hoof health, gender and more.
But I’m getting ahead of myself. For those unfamiliar with Chronic Progressive Lymphedema (CPL), here’s the Cliff's Notes. Before CPL became the mainstream terminology for this condition, it was often referred to as Chronic Pastern Dermatitis (CPD) or Chronic Proliferative Pastern Dermatitis (CPPD) - a term still used by vets across the USA and Canada. In 2003, the syndrome was redefined as Chronic Progressive Lymphedema (CPL), mainly because of its similarities to the clinical presentations within the human condition, which we know as chronic lymphedema. It should be noted that this is a bit misleading for horse owners, given that equine chronic lymphedema (CPL) symptoms are assumed to occur secondary to, or as the result of, CPD. I need to restate here that there is presently no causation and manner of disease development of CPL to date, so all of this is just theory.

No matter the accuracy of the term CPL, let me break down what CPL is exactly. It’s said to be a multifactoral disease that occurs in several heavy draft horse breeds, light drafts and some draft horse crosses. Typically, clinical symptoms start in the lower limbs and include progressive soft tissue swelling and fibrosis (thickening or scarring of the tissue) along with the development of skinfolds and nodules. Skin issues may include excessive scaling and ulcers. Secondary conditions can sometimes develop as a consequence of primary CPL lesions.
Additionally, hyperkeratotic skin provides an ideal environment for mites, which triggers a chain of events leading to the onset of CPL. For example, mites aggravate the skin, so the horse scratches the itch. In the process of aggressively biting their irritated leg, they break the skin and bacteria infiltrates the wound. The skin becomes inflamed as a result and that prolonged inflammation impedes the lymph drainage system. Since a dysfunctional lymphatic system directly impacts the skin’s ability to fight infection, bacteria grows and spreads. As infection worsens, the leg swells even more. Swelling causes the skin to crack and flake dead skin, which is the mites’ absolute favorite meal. Mites settle in, reproduce and the vicious cycle continues. Between the skinfolds, dirt and moisture can accumulate, creating opportunities for secondary bacterial or fungal infections. These secondary skin infections can produce foul smelling exudate (fluids) and ulcers. Flies are attracted to the stink and in some worse-case-scenarios, maggot infestations have occurred.
"CPL is 86% environmental and 14% genetics," says Dr. Marieke Brys. That means the way a horse is fed, their activity level, where/how they live, their preventive mite care, grooming, all of it, factors 86% of whether the horse will develop and/or progress with CPL symptoms and how severe those symptoms will become.
The speed of CPL progression is largely dependent on additional influences such as hygiene, skin care, secondary infections and trauma. Lymphedema will have an effect on the dermis, subcutis and tissues in the distal legs. In more advanced stages, dermal thickening can be so severe that it encloses the entire leg, typically at the level of the joints, resulting in a restriction of the horse's movement. This can cause a certain degree of lameness. In the most extreme cases, humane euthanasia is required.
CPL has been observed in several breeds a to include, but not limited to Brabants, Shires, Clydesdales, Gypsy Cobs and Vanners, Friesians, American Belgians, Ardennes, Bréton, Boullonais, Cheval Trait Auxois, Percheron, and German draft horse breeds such as the South German, Black Forest, Schleswig, Saxon-Thuringian, German Rhenish and Mecklenburg. One study estimates over 85% of the Brabant breed is affected, while another study estimates it more conservatively at around 60%. Either way, why is CPL happening?
Again, it’s theorized that CPL has an unidentified genetic component and breeds with limited breeding numbers, like many draft breeds, demonstrate a higher incidence of CPL due to the recirculated gene pool. Based on this theory, for Brabants it’s a numbers game. According to Trekpaard.net, the current number of Brabants in Belgium are roughly 5,000 horses with an estimated 550 foals born annually. That’s crazy considering the breed boasted 278,000 horses in Belgium at the turn of the 20th century. But that’s what two World Wars and the invention of the tractor will do to a breed. At any rate, due to the plummeting numbers threatening the extinction of the Brabant, several European associations were established in order to preserve and promote what was left of the beloved, but decimated breed.

A byproduct of having very few breeding horses to keep the breed going early on was inbreeding. With a present-day CPL incidence rate somewhere between 60-85% of all Brabants, it’s safe to assume a genetic predisposition was carried forward from those foundation draft horses all those years ago. The very same gene which is now theorized by some to be the cause of CPL onset (more on the skin sensitivity theory later).
"In small populations, the choice of mates is also limited. Over time, individuals will all become related and will be forced to mate with relatives. This is inbreeding. Inbred animals often have two identical alleles for their genes because the same gene was passed on from both parents. If this allele has harmful mutations, an inbred baby can be unhealthy," Dr. Melissa Minter, Ph.D. researcher at the University of York, United Kingdom.
Today, European associations have been working toward breeding out CPL. Two methods of selection against CPL are phenotypic selection and estimated breeding value (EBV) selection (read up on EBV). Essentially, EBV provides the measurement of the breeding potential of an animal for a specific trait. They take into account performance data collected on known relatives, the relationships between performance traits (correlations) and the degree to which traits are inherited from one generation to the next (heritabilities). The European studbooks adopted the phenotypic selection, which presently evaluates and scores breeding stallions’ legs during annual stallion inspections.
"Phenotical breeding has been largely ineffective in reducing incidence of CPL," says Dr. Brys. "That has been proven here in Belgium over years and years of scoring and selective breeding based on the stallion's legs. A better approach would be to assess the stallion's offspring."
However, a recent study has shown this approach has not been substantially effective. As Dr. Brys pointed out above, CPL has a low to moderate heritability (14-26%), resulting in a low efficiency of phenotypic selection, therefore some say EBV’s would likely render better results.
As an aside, we at European Brabant Registry of America (est. in 2021) face the same breeding challenges on this side of the Atlantic. In some respects, it’s even more difficult as the purebred Brabant is more rare in America.
"If genetic diversity gets too low, species can go extinct and be lost forever," says Dr. Melissa Minter. "This is due to the combined effects of inbreeding depression and failure to adapt to change. In such cases, the introduction of new alleles can save a population. This is called genetic rescue (A conservation strategy where new individuals are introduced into a population to increase genetic diversity and improve population health.)"
In an effort to avoid inbreeding and to broaden the gene pool, the European Brabant Registry of America (EBRA) developed the “Breed Up” program (read more here) where breeders have the ability to selectively cover outside phenotypic draft breeds with purebred Brabants and “Breed Up” to the purebred threshold of 15/16, or 93.75% European Brabant bloodlines. These qualifying “Breed Up” Brabants are then evaluated and scored against breed standards by a panel of independent judges. Those who pass inspection are included in the EBRA’s premier purebred European Brabant Studbook. This program allows us to preserve the heritage of the Brabant breed, while also introducing fresh, outside blood to the genetic mix. As Dr. Minter noted above, genetic diversity improves the overall health of any species. It should be noted again, that many heavy draft horses are susceptible to developing CPL so even this approach may not be effective in breeding out CPL. Only time will tell. All we can do at the EBRA at this time is help contribute to research and studies, suggest best prevention and treatment practices within our Brabant community and reduce inbreeding through the Breed Up Program and our Grassroots “Test A Mating” app, where EBRA Members can virtually pair Brabants to see if there are any overlapping bloodlines.

Now why does CPL start in the first place? To date, there’s been a lot of theories and speculation, but nothing concrete. That’s where Marieke Brys, Master of Veterinary Medicine at the University of Ghent, study comes into the picture. Marieke dedicated two years of study to CPL and wrote a dissertation titled, “Chronic Progressive Lymphedema in Draft Horses: ‘Mites or Myth?’.” She has committed another six years of her life to the continuation of her CPL study. As the owner of a Brabant mare with CPL, she sought answers on how to care for and treat her horse, but noticed a gap from the study of the disease to any viable recommendations regarding treatments for the condition. After pouring over all available resources from science-based research to Facebook CPL groups and talking with equine lymph drainage practitioners and supplement developers, Marieke landed on the mite theory. She suspected that non-burrowing mites, Chorioptes Bovis, or C. Bovis for short, are what ignite a chain reaction leading to the onset of CPL. Her hypothesis was that If she could eradicate the infestation, she could begin to heal her mare’s legs.
In draft horses, a remarkably high prevalence of mites has been described in several studies, ranging from 50% up to 95%. As described in my previous example, these C. Bovis mites cause itchy skin, scaling and crusting of the distal limbs and this skin scaling and epidermal debris in-turn provides an abundant food supply for the mighty mites. Not only is there ample food, but the feathers provide shelter from the elements too. Essentially, draft horse feathers are the penthouse of mite real estate. So Marieke eliminated the mites’ shelter by clipping her mare’s feathers. She then exterminated the infestation by applying Cydectin (currently not approved for use in horses) at marked intervals to cut-off the lifecycle of the mites.
For safety purposes, do not attempt this treatment without the guidance of a licensed veterinarian. Foals and yearlings should never be treated with Cydectin. Just like parasites becoming resistant to dewormers, there is a potential for mites to become tolerant to topical treatments.
Over time, her mare’s legs improved; swelling reduced significantly and the sores healed. Her mare no longer scratched and stomped. To reinforce her theory, she expanded the study to other CPL affected horses - establishing a placebo-controlled approach. Once again, the same promising results. As I mentioned before, she is continuing this study and expanding her research to include biopsies so she can further study the long term impacts of CPL on horse’s lymphatic system and skin.
Marieke says that the dysfunction of the lymphatic system, fibrosis, inflammation, and an aberrant elastin network are the four factors that appear to be associated with CPL and provide the basis for her hypotheses. But the timeline of these events is not clear, she says. For example, lymphedema can cause inflammation and fibrosis. Conversely, chronic inflammation can also cause a malfunctioning lymphatic system, she elaborated. A vicious circle can be created where these factors might permanently reinforce each other, therefore no trigger factor for this condition has yet been identified. Consequently, several diverging hypotheses have been formulated regarding the cause of this disorder.
“I believe it is possible that current hypotheses are not independent of each other,” she said, “Rather, each may explain part of the disorder development. The genotype-environmental interaction is defined as a different effect of a certain genotype on disease risk in animals with different environmental exposures.”
The EBRA hosted a virtual CPL clinic with Dr. Marieke Brys and EBRA Members can stream her program videos on the Forum now! CLICK HERE to tune in.
Again, there is currently no curative treatment for CPL. So what can we do? At this point, careful management and supportive therapy can improve the quality of life of affected horses. These treatments can be labor intensive and must be carried out during the whole lifespan of the horse to minimize discomfort, slow the progress of the disease, and avoid recurrent infections. These treatments focus primarily on wound and skin care, prevention of secondary infections and additionally on controlling tissue edema. Here are a few ways to organically support a horse who is predisposed to, or who has CPL. I've broken these tips down by the horse's environment, the horse's diet and the horse's leg care.
ENVIROMENT:
Provide room to roam. Standing still or in confined spaces without the ability to move is detrimental to the health of the equine lymphatic system. Whenever the horse is standing and unable to flex its fetlock joint fully, the mechanical retraction apparatus for removing the lymph from the lower limb is compromised. If possible, increase the level of turnout or find ways to encourage the horse to walk more.
Install a track system. For track system ideas, check out Jamie Jackson's Paddock Paradise.
Reduce wet areas in pastures such as high traffic paths, shelters, and water troughs by installing mud management grids and/or gravel.
Warning: Horses should never be fed on gravel as they can ingest it leading to colic or tooth damage.
Have a well-defined and strictly enforced exercise program that includes daily or near-daily structured exercise, even if it is low-intensity work such as trail riding or in-hand walking.
Start all work, whether under saddle or in harness, with a long warm up and a long cool down period.
Provide shade from strong sunlight. If possible, provide a fan during the hottest times of day. For horses with white legs, use SPF 50-60 sun block to protect un-pigmented areas during sunny weather.
Control biting insects. Hang fly control bags/strips and apply a good fly repellent. Spray the entire skin including the affected limb(s), the underside of the belly, sheath and teats.
Mites thrive in straw, so choose an alternate bedding such as shavings and/or rubber floor mats. Shavings can hold moisture, so they too have pitfalls.
Do not use leg wraps or boots that will retain moisture. Do not share boots between horses.
Keep horses barefoot when possible. Regular farrier care is critical for horses with CPL as their hoof quality may be compromised due to the lymphedema involved. Cleaning the hooves daily is important to check for the development of thrush.
DIET:
Provide access to free choice hay or fibre. The lymph vessels need the peristaltic action of the intestines to help them move. If worried about weight gain, try slow feeders and/or soaking the hay to remove nutrients prior to feeding or take advice from your vet or qualified nutritionist.
Forage can be supplied as pasture, hay, or hay alternatives such as pellets or cubes. Well-maintained pastures should contain low-sugar grasses and no legumes (ie: clover, alfalfa or lucerne). Grazing areas should not be lush, and low-yield acreage—one step above a drylot—seems to be especially suitable.
If you’re unsure about pasture suitability, pasture grasses can be analyzed by a reputable laboratory to determine if nonstructural carbohydrate (NSC) levels are less than 12%, which seems appropriate for most draft horses.
In addition to the nutritional advantages of turnout, foraging allows for an increase in exercise, which is essential for draft horses.
For times when too much forage is available, a grazing muzzle can limit intake.
Hay and alternative hay sources such as pellets and cubes should be made from grasses and should also have NSC levels less than 12%. Appropriate hay is often mature and in most cases should be selected over more energy-dense immature hay, though all hay should be free of mold, dust, and foreign material.
If a horse requires additional calories to maintain weight while exercising and/or breeding, a concentrated source of energy should be offered. Neither straight cereal grains such as plain oats nor textured or sweet feeds containing cereal grains should be fed.
A low-starch, high-fat feed formulated provides adequate energy to horses in the form of alternative energy sources such as fermentable beet pulp and vegetable oil.
Horses on all-forage diets require vitamin and mineral supplementation for optimal health. A ration balancer will make up for any shortfalls in protein, vitamin, and mineral nutrition, and will not add significantly to the NSC content of the diet. Most ration balancers are designed to be fed at a rate of 1-2 lb (0.45-0.9 kg) per day.
In lieu of a ration balancer, a well-fortified vitamin and mineral supplement, such as can be fed if even 1 lb (0.45 kg) of a balancer pellet is too many calories for the horse. Look for Micro-Max in the U.S.
For certain horses, additional calories in the form of vegetable oil might be necessary. In light of the benefits proffered by omega-3 fatty acids, choose soybean or canola oil, as these are richer in omega-3s than corn oil. Between 100 and 500 ml (0.25-2 cups) of oil can be fed daily, though it should be added gradually over a period of a week or so.
Add herbs such as Hilton Herbs immune support and lymph support.
Provide a vitamin E supplement, the most potent of which is a natural, nanodispersed product called Nano-E. Vitamin E should be offered at an intake of 1-1.5 IU per ml of supplemental oil in addition to 2-3 IU of vitamin E per kg body weight for horses in light work. A 1,100-lb (500-kg) horse, for example, should receive 1,000-2,000 IU of vitamin E per day.
In addition to its antioxidant responsibilities, vitamin E is vital to immune, cardiovascular, circulatory, neuromuscular, and reproductive functions.
LEG CARE:
Keep the feathers clean! Use a soft, antimicrobial brush like the Vale Dandy Brush to keep the hair loose and dry. Apply some Coat Defense daily preventive powder to keep hair while reducing fungus and bacteria.
Test the brush to ensure softness. Use the brush on the inside of your arm and if your skin turns pink or it feels sore, don't use it.
If you can't keep the feathers clean or don't have the time to provide routine care, or your horse has open sores, clip the feathers.
After clipping leg feathers, apply a water based antiseptic cream (hydrogel) twice a day for for ten days to hydrate and protect the skin. This will also treat any nicks or cuts caused by the clippers.
If the feathers are muddy, wash them using room temperature water (never hot or cold as this can impact lymph flow). Don't use rough brushes or scrubbers to break the mud loose as these may break the skin, cause more irritations and leave the skin more open to bacteria and infection. Use a non-drying, soothing shampoo with essential oils like E3 Tea Tree or Coat Defense Shampoo.
If legs have open sores, use an antibacterial/anti-fungal shampoo like E3 or Chlorhexidine Scrub to clean the legs. These shampoos can dry the skin, which can be detrimental so use these products sparingly.
When using these, shampoo the area once or twice daily for seven to 10 days, lather, leave on 10 minutes, rinse and pat dry well. Then decrease the frequency to two to three times weekly. If lesions ooze exudate, apply astringent solutions, such as lime sulfur or aluminum acetate.
If skin is already very dry, use a cream wash to clean the legs. Using an emollient cream like Epaderm or Eucerin. Apply to the leg in the same way as you would a soapy lather, gently rinse and then pat dry using clean microfibre towels. The cream will help remove mud and particles but won't dry the skin like shampoos or antimicrobial soaps.
"Getting thorough saturation when applying Lime Sulfur Dip can be challenging, whether the horse has feathers or not," explains Stacy Pearsall, (EBRA Member V0003). "I use a Ponyjet hose attachment which allows me to pour a measure of Lime Sulfur Dip solution into the nozzle's reservoir and water dilutes the concentrate as it's sprayed onto the horse's legs."
It is also important to avoid the use of elasticated products to the lower limbs, as there is no musculature to guard against over-compressing the deep lymphatic collector vessels. These vessels are very vulnerable to being constricted and research has shown examples where elastic bandages have effectively cut off lymphatic circulation.
Here are other treatments that should be performed by licensed practitioners and/or veterinarians:
Diligent management can improve the quality of life for horses with CPL, although there is no cure for the condition, says Jamie Thomas, Bachelor of Science.
Resources and References
https://pubmed.ncbi.nlm.nih.gov/24267676/
https://pubmed.ncbi.nlm.nih.gov/18052806/
https://pubmed.ncbi.nlm.nih.gov/24267677/
https://pubmed.ncbi.nlm.nih.gov/31908060/
https://pubmed.ncbi.nlm.nih.gov/2275309/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7152136/
https://libstore.ugent.be/fulltxt/RUG01/003/061/127/RUG01-003061127_2022_0001_AC.pdf
https://lib.ugent.be/catalog/pug01:4092334#reference-details
https://pubmed.ncbi.nlm.nih.gov/21592216/
https://pubmed.ncbi.nlm.nih.gov/33389135/
https://pubmed.ncbi.nlm.nih.gov/4071949/
https://pubmed.ncbi.nlm.nih.gov/15624437/
https://pubmed.ncbi.nlm.nih.gov/16808668/
https://pubmed.ncbi.nlm.nih.gov/16536384/
https://pubmed.ncbi.nlm.nih.gov/19147156/
https://pubmed.ncbi.nlm.nih.gov/24641331/
https://pubmed.ncbi.nlm.nih.gov/25500056/
https://pubmed.ncbi.nlm.nih.gov/24593274/
https://pubmed.ncbi.nlm.nih.gov/24641331/
https://openjournals.ugent.be/vdt/article/id/75602/
https://pubmed.ncbi.nlm.nih.gov/21539228/
https://pubmed.ncbi.nlm.nih.gov/22558778/
https://pubmed.ncbi.nlm.nih.gov/17910266/
https://pubmed.ncbi.nlm.nih.gov/17910261/
https://pubmed.ncbi.nlm.nih.gov/16964652/
https://pubmed.ncbi.nlm.nih.gov/26753358/
https://www.regulations.gov/document/FWS-R4-ES-2014-0065-0208
https://pubmed.ncbi.nlm.nih.gov/16124697/
https://pubmed.ncbi.nlm.nih.gov/16359304/
https://pubmed.ncbi.nlm.nih.gov/16359304/
https://pubmed.ncbi.nlm.nih.gov/11558745/
https://pubmed.ncbi.nlm.nih.gov/20181429/
https://pubmed.ncbi.nlm.nih.gov/20609205/
https://pubmed.ncbi.nlm.nih.gov/29132848/
https://apvma.gov.au/sites/default/files/publication/14406-macrocyclic-lactones-review-report_.pdf
https://pubmed.ncbi.nlm.nih.gov/9224211/
https://chronicprogressivelymphoedema.com/chronic-proliferative-pastern-dermatitis/
https://www.facebook.com/CPLPAGE/
https://pubmed.ncbi.nlm.nih.gov/33830562/
https://www.vet-ebooks.com/pascoes-principles-and-practice-of-equine-dermatology-2nd-edition/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3981917/
https://pubmed.ncbi.nlm.nih.gov/32534850/
https://pubmed.ncbi.nlm.nih.gov/11951782/
https://pubmed.ncbi.nlm.nih.gov/22076327/
https://pubmed.ncbi.nlm.nih.gov/7701306/
https://pubmed.ncbi.nlm.nih.gov/12054136/
https://pubmed.ncbi.nlm.nih.gov/20039044/
https://pubmed.ncbi.nlm.nih.gov/17395600/
https://pubmed.ncbi.nlm.nih.gov/23517354/
https://beva.onlinelibrary.wiley.com/doi/abs/10.1111/j.2042-3292.2004.tb00272.x
https://pubmed.ncbi.nlm.nih.gov/15954550/
https://pubmed.ncbi.nlm.nih.gov/15945386/
https://pubmed.ncbi.nlm.nih.gov/20178503/
http://europepmc.org/article/MED/20067360
https://pubmed.ncbi.nlm.nih.gov/21827555/
https://pubmed.ncbi.nlm.nih.gov/17827472/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3780325/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8360305/
https://pubmed.ncbi.nlm.nih.gov/27219461/
https://pubmed.ncbi.nlm.nih.gov/2252623/
https://www.elsevier.com/books/equine-dermatology/scott/978-1-4377-0920-9
https://pubmed.ncbi.nlm.nih.gov/7483237/
https://pubmed.ncbi.nlm.nih.gov/34644903/
https://pubmed.ncbi.nlm.nih.gov/19725269/
https://www.trekpaard.be/nl/nieuws/Brabants-trekpaard-met-uitsterven-bedreigd
https://www.trekpaard.net/nl/over-ons
https://vilt.be/nl/nieuws/brabants-trekpaard-immaterieel-cultureel-erfgoed-1
https://biblio.ugent.be/publication/524962
https://pubmed.ncbi.nlm.nih.gov/15046463/
https://pubmed.ncbi.nlm.nih.gov/16943065/
https://pubmed.ncbi.nlm.nih.gov/25180696/
https://pubmed.ncbi.nlm.nih.gov/16884936/
https://www.frontiersin.org/articles/10.3389/fimmu.2019.00076/full
https://beva.onlinelibrary.wiley.com/doi/10.1111/evj.12256
https://www.worldhorsewelfare.org/advice/health/how-do-you-treat-mites-in-horses
https://ker.com/equinews/diet-adjustments-provide-relief-pssm-horses/
https://pubmed.ncbi.nlm.nih.gov/11243365/
https://pubmed.ncbi.nlm.nih.gov/11759989/
https://pubmed.ncbi.nlm.nih.gov/14567431/
https://pubmed.ncbi.nlm.nih.gov/16379634/
https://forums.horseandhound.co.uk/threads/chronic-progressive-lymphedema-cpl.354468/
https://drjendvm.wordpress.com/2010/06/17/chronic-progressive-lymphedema/
https://www.mdpi.com/2076-2615/10/3/542
COMMON SKIN CONDITIONS
Article Researched and Written by Stacy Pearsall (See References)
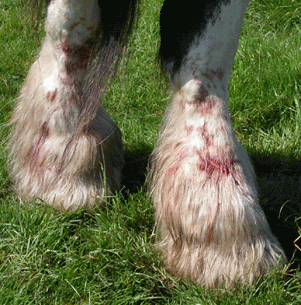
Above images from left to right: Mud Fever, Scratches, Mange, Dandruff, Mallenders Sallenders. (For Image Sources, See References)
Hopefully you've read the previous article on CPL and have a better understanding of what it is and what to look for. There are several common skin conditions that are correlated with the early clinical signs of CPL. That said, a horse with any of these conditions does not necessarily mean they have CPL. However, given what is known about CPL, the prevention and/or treatment of these common skin conditions can help avert the triggers and/or progression of CPL. Please note: The treatment products provided are used as a reference only and should not be seen as an endorsement by the EBRA. Be sure to consult with your vet before using any of these products.
MUD FEVER: A wide range of skin conditions known as pastern dermatitis or pastern folliculitis. In addition to the nickname "mud fever", it's also known as "scratches", "dew poisoning", "greasy heel" or "cracked heels". No matter the name, this mixed bacterial, often fungal, and sometimes parasitic skin condition is a major pain. It can be caused by a variety of bacteria, which thrive in muddy, wet conditions. The infection can stay dormant in the horse’s skin and only become active when the surface is compromised, usually by prolonged exposure to wet conditions. If a horse does get mud fever, the signs you may see are quite distinctive and include matted areas of skin containing crusty scabs, with lesions beneath. There is often a thick discharge between the skin and the overlying scab. You may also notice heat and swelling, with the horse reacting to pressure or flexion of the affected limb. Eventually, hair loss can leave inflamed, raw-looking skin which may split open at the back of the leg in severe cases, creating the horizontal fissures characteristic of cracked heels.
Any horse can get scratches, but the condition is widely prevalent in draft horses with feathers or long fetlock hair that retain moisture. Horses with white legs are also at risk because un-pigmented skin is more susceptible to sun damage, chaffing and abrasions making it more at risk for infection.
If you know your horse is prone to mud fever, it’s important to keep their legs as dry as possible. Try to prevent your paddock from getting badly churned up, as the bacteria are transmitted in the soil. If it’s possible, changing the point at which you enter the field and moving water troughs regularly can be helpful.
Cover particularly muddy areas with sand.
If your best efforts don’t succeed, you'll need to treat the infected area. Clip away the feathers, taking care not to scrape or break the skin. Once the area is clipped, gently wash the affected areas with an antibacterial shampoo or an antifungal shampoo (1-2% miconazole) and let it sit for about 10 minutes before gently rinsing. Rough scrubbing and harsh chemicals should be avoided. Scabs can be massaged off carefully, but don't pull or pick them. Using a clean towel, carefully pat the area dry and apply a topical treatment. Limit washing sessions to only once a day for 7-10 days. Then cut back the frequency to 2-3 times per week until resolved.
MANGE (MITES): Mange is a parasitic infection caused by several species of tiny mites that can barely be seen by the naked eye. The most common form that occurs in horses in the United States is chorioptic mange, caused by the mite Chorioptes equi, which typically affects the lower legs of horses with feathering. Although rare, horses may also develop psoroptic mange (Psoroptes equi), which produces lesions under the mane and tail, under the jaw and in the groin and armpits, and demodectic mange (Demodex equi), over the face, neck and shoulders. Presents as small, round bumps at first, soon followed by bald spots, with scaly, thickened skin, usually on the lower legs of draft horses with heavy feathering, although any horse can be affected. In more serious cases the skin may be rubbed raw and show signs of secondary infections. Mange causes itching, and horses will rub, stamp and bite at their legs. In rare cases, mange may appear on other parts of the body.
A number of topical antiparasitic products can be effective against mange—look for products that contain lime-sulfur solutions, organophosphates or permethrins, which can be applied by spraying, sponging or dipping the leg.
Administering oral ivermectin or moxidectin may also be helpful in some cases. Treatments may need to be repeated three or four times at 12- to 14-day intervals.
Clipping the legs will help the topical treatments reach the skin but may not be necessary in all cases, especially if the infection is still mild.
Mites usually are passed directly from horse to horse, so do not allow your horse to have contact with others at shows or events and quarantine newcomers on your farm, especially if they have visible bald areas that appear to be itchy. Some horses can carry the mites without showing signs of infection and can be a source of recurrence after other horses are treated. If you have an outbreak, it’s a good idea to treat all horses who have been in contact with the ones affected and change out all of the stall bedding used by affected horses.
SKIN ALLERGY: Reddened skin and / or hives are a common result of an allergic reaction. Just like people, many different substances can cause an allergic reaction in a particular horse. It could be something that touches their skin, something they breathe, something they eat or even a new medicine or vaccination from the vet. Allergic reactions can be one of the more frustrating skin conditions on horses because it can be complicated and difficult to diagnose. Many horses are severely allergic to the saliva from bites of insects – especially small gnats, sometimes called no-see-ums. The resulting welts and irritated skin is often referred to as “sweet itch.” The horse will scratch themselves constantly resulting in lesions. Sweet itch often shows up in fly season along the top-line of the horse or the tail dock area.
If your horse is having a severe attack, or symptoms are worsening, your veterinarian may decide to administer a cortisone shot or other treatment to lessen the effect of the allergen.
In the long term, treating an allergic reaction presenting in a skin condition is best done by figuring out what is causing it, then removing that factor completely from your horse’s life. Work closely with your veterinarian and provide them with as much information as you can.
An allergic reaction often happens within a few days of the horse being exposed to the allergen. Try to think of anything new that your horse has touched, breathed, eaten or been treated with. It can be as subtle as a change in brands of a horse care product, tack or bedding. Or it may be something that is brand new to your horse care regimen.
MALLENDERS AND SALLENDERS: Sallenders occurs in the crease of the knee on the front leg and Mallenders is present in front of the hock on the hind legs. It can be identified by the thickened, crusted scale and scabs on the front and hind legs of horses. Sallenders and Mallenders can become extremely uncomfortable for your horse and if left untreated can cause secondary fungal and bacterial infections that lead to lameness. The cause of Sallenders and Mallenders is the overproduction of keratin, the building block of hair, horn and that beautiful, luxurious feather. There is no cure for Sallanders and Mallanders but it can be managed easily.
Wash: The risk of a secondary infection has to be limited as much as possible.
Ointment: Applying a moisturizing ointment to keep the area from drying out and producing more cracks, is recommended.
Don't Pick: As tempting as it may be – do not pick at the scabs. Allowing the ointment to soften the scabs and fall off by themselves, is still the safest way to get rid of it.
DANDRUFF: Seborrhea, or dandruff, can be dry or oily. In the dry form, small flakes of skin appear routinely, usually at the base of the mane and tail, and sand-like flecks may appear on the girth area or anywhere sweat accumulates. Oily seborrhea causes large, waxy crusts, often on the elbows, hocks or lower legs; when peeled off, these may leave hairless patches up to several inches in diameter. Dandruff sometimes causes a fetid odor, but the horse is not usually itchy or in pain.
Primary seborrhea is not curable, but it can be managed. A number of antidandruff shampoos are available that, when used as directed, can dissolve flakes and loosen oily scales.
It’s best to choose products formulated for use on horses; human products can be too harsh.
Gentle scrubbing with a soft- to medium-bristled brush can help remove crusts.
If you have difficulty controlling a stubborn case, talk to your veterinarian, who may recommend other topical medications.
Resources
https://equusmagazine.com/horse-care/common-equine-skin-diseases/
https://eliteequineuk.com/blog/mallanders-and-sallanders-in-horses/
https://equiderma.com/skin-condition/mallenders-and-sallenders-hyperkeratosis/
https://www.mannapro.com/equine/itching-for-spring-learn-to-identify-treat-horse-skin-conditions
https://www.severnedgevets.co.uk/equine/advice/under-skin-truth-about-mud-fever
https://absorbine.com/pages/identify-treat-prevent-skin-conditions-on-horses
https://towcester-vets.co.uk/article/preventing-identifying-treating-mud-fever-in-horses/
https://www.banixx.com/scratches-injuries-horse-how-to-treat/
https://horselifeandlove.blogspot.com/2016/06/all-about-mange.html
https://www.mcgeeequine.com/services/dermatology/
PREVENT THE SPREAD
by Stacy Pearsall
There are communicable diseases amongst horses that can be spread easily by community-use brushes, collar and saddle pads, turn-out blankets, harness and even halters. Here are a few of those pesky pestilence:
Rain rot, or bacterium Dermatophilus congolensis, are small, round scabs crowned with matted hair. These lesions typically develop along the topline of the horse. Rain rot is contagious and zoonotic, which means that other horses and humans can contract the condition.
Pastern dermatitis, or scratches, is a name for a clinical syndrome, rather than a specific disease. It is the development of scabby areas on or near the pasterns. The two most common causes of pastern dermatitis include bacterial infections and mange. Mites can also cause pastern dermatitis in horses with feathers, they spread from horse to horse and can survive in the environment for several weeks.
Ringworm is a skin infection caused by a dermatophyte (skin 'loving') fungus of which there are several different species. The fungi which causes ringworm in horses include the Microsporum and Trichophyton species, is contagious amongst horses and zoonotic.
Reduce the incidence of spread by applying these cleaning practices quarterly, or monthly if needed:
Grooming Tools & Nylon Halters: Remove all hair build up from brushes. Wash all brushes, combs, curries, sweat scrapers, hoof picks and other grooming tools with Dawn dish soap in warm-to-hot water to clean away skin oils, dirt and debris. You can scrub brushes against each other to help break loose stubborn build up. Let everything thoroughly dry, before disinfecting with a bleach solution (3/4 cup bleach per gallon of water). Remember, when dish soap and bleach interact a toxic gas is produced. Let everything sit in the bleach solution for at least thirty minutes. I actually let mine sit overnight. Rinse everything thoroughly and let dry.
Tip: Wear gloves when handling bleach.
Tip: Use a storage bin with lid as your wash basin.
Saddle Pads, Collar Pads & Blankets: Start by removing as much debris, dirt and hair as possible, using a horse brush and/or vacuum. If blankets are machine-washable, run them through the wash cycle with Lysol disinfectant rather than bleach (1 cup in a standard top-load washer). Spin dry and run through a second wash cycle with a small amount of regular laundry soap. Air-dry pads and blankets completely, ideally in direct sunlight.
Tip: If your washing machine is too small, or you don't want to bring barn gear into your house, use a storage bin with lid as a wash basin. Add hot water and Lysol solution, close the lid, soak for ten minutes and agitate for one minute. Periodically open the lid then lift and plunge the item in and out of the water a few times before closing the lid and repeating the soak and agitation process. Rinse thoroughly, then air dry.
Leather and Biothane Harness & Halters: There is no dedicated disinfectant spray specifically for leather but Lysol, when diluted, is a safe disinfectant for leather. Beware, Lysol is an alcohol-based disinfectant, and there is a strong chance it can dry out or discolor leather if not applied properly. Start by thoroughly cleaning the tack then apply diluted Lysol solution (1 part Lysol to 5 parts water) using a soft cotton towel or rag. Never directly spray solution to tack. Completely dry the tack's surface after applying the Lysol disinfectant to reduce incidence of discoloration or dry out.
Personal Outerwear: You may be ground zero! Don't forget to apply the disinfectant process to your gloves, jackets, overalls and other items too.
For all those in-between times, I suggest having a can of Lysol Fabric Disinfectant Spray and a spray bottle with dilute Lysol in the barn, so you can spot treat your gear after you finish working horses. Just be sure to let the gear dry before using them on another horse.
It goes without saying that all disinfectants mentioned above are for use on tack and grooming gear only and should not be applied to or ingested by horses as treatment. Be sure to keep track of the detergents and cleaning products that you do use, just in case your horse develops a condition after tack and equipment is cleaned and used. Discuss this development with your vet.
















































Comments